First Aid Techniques for Choking

If a patient is choking and is unable to breathe, cough, or speak, Home Health Aides/Personal Care Aides must take immediate action and call 911. Permanent brain damage could occur in as little as four minutes if the person is unable to breathe.
- Try to encourage them to cough to remove the object or food.
- Stay with them at all times while you are waiting for help.
- Use your senses of observation to determine the cause and extent of the choking. Did the person swallow an object or did the choking happen while they were eating, drinking, or taking medicine? Are they able to breathe? Are they turning blue (cyanotic)? Do you hear soft or high pitched sounds when they are trying to breathe? Are they unable to make any sound or cry? Are they unable to cough or is the cough weak and ineffective (not working)?
Heimlich maneuver
If needed, Home Health Aides/Personal Care Aides must be prepared to perform abdominal thrusts to help dislodge the object from the person’s airway. This method is called the Heimlich maneuver. Remember to only do this if the person cannot breathe, cough, or speak. Ask if they need help and if they are choking prior to performing abdominal thrusts.
Performing the Heimlich maneuver for a person who is standing or seated:
- Stand behind the person and wrap your arms around their waist.
- Make a fist with one hand, and place your thumb against the person’s abdomen, just above their belly button.
- With your other hand, grasp the fist that is against their abdomen and quickly and forcefully thrust both hands up toward you.
- You should be thrusting inward and upward. This helps to move the object out of the person’s airway.
- Repeat this until the object becomes dislodged, or if the person loses consciousness.
- If the person loses consciousness, lower them to the floor and begin CPR if trained to do so.
- Keep the person in a lying up position so that their head is facing up.
- Ensure their airway is not blocked.
Performing the Heimlich maneuver for a person who is in a lying position:
- If the person is in a lying down position and begins to choke, straddle them, facing their head.
- Grasp your fist as you would if they were standing.
- Push upward and inward to help dislodge the object.
- Ensure their airway remains free and they are in a face up position.
Performing the Heimlich maneuver in an infant:
Performing abdominal thrusts on an infant is a different process.
- Lay the infant face down on your forearm, across your lap or thigh.
- Provide support to his or her head and neck by placing your one hand under their chin to hold it steady.
- The baby’s head should be facing downward, lower than their body. This helps to provide gravity so the object can be removed.
- Using the bottom (palm) of your other hand, provide 5 blows to the baby’s back, between the shoulder blades.
- If the object becomes dislodged, you can stop.
- If the object is still stuck, turn the baby face side up.
- Provide support to his or her back with your forearms, resting the baby on your lap or thigh.
- Provide 5 chest thrusts by using 2 fingers in the center of their breastbone and quickly press down, compressing their chest about 1/3 to ½ the depth of their chest.
- You can repeat this process until the infant expels the object or until they lose consciousness.
- Remember, 5 back thrusts with the baby face down, and then 5 chest thrusts with the baby face up.
Document all instances of choking and steps taken to provide care. The supervisor should always be informed about any instances of choking.
First Aid Techniques for Poisoning
If Home Health Aides/Personal Care Aides suspect or know that poisoning has occurred, they should try to determine the source of the poison. This is important information which they will need to provide to Poison Control in order for them to best help. Look for nearby medications, chemicals and cleaning solutions that the patient may have ingested. Immediately call Poison Control and follow their directions. The treatment for poisons depends on the type of poison that was ingested. Notify a supervisor as soon as feasible. Never try to make a patient vomit, unless specifically instructed to do so. Some chemicals may cause severe harm if they come back up the esophagus during vomiting. Document all poisonings and steps taken to provide care.
What to do in Serious Medical Emergencies
Should a serious medical emergency occur, Home Health Aides/Personal Care Aides should assess the situation using their observational senses. Note what is seen, heard, felt, and smelled. Immediately call for help. Activate emergency medical services (EMS) by dialing 911. Inform them in a calm and matter of fact way what occurred and the observations made. Never leave the victim unattended.
Keep in mind the ABCs of first aid. The ABCs of first aid stand for A (Airway), B (Breathing), and C (Circulation). It is important to remember this acronym as any delay in treatment when a patient has a compromised airway, breathing, or circulation could result in serious injury, and possibly death.
Assessing the ABCs
Airway
Is the patient’s airway (mouth, nose), open? Is there an obstruction which makes it impossible for them to breathe? If there is an obstruction and the person is unable to breathe, activate EMS and perform the Heimlich maneuver to try to remove the obstruction.
Breathing
Is the person breathing? Can you see the chest rise and fall as they breathe? Can you feel air move in and out of their mouth or nose? If the answer is no to any of these questions, Home Health Aides/Personal Care Aides should activate EMS and begin CPR if trained to do so.
Circulation
Do they have a pulse? How is their color? Are they blue from lack of oxygen? Does their skin feel warm to the touch or cold? Cold skin means not enough blood is pumping through the body. If the person does not have a pulse, Home Health Aides/Personal Care Aides should activate EMS and perform CPR if trained to do so.
Take note of the ABCs of first aid. Activate emergency medical services if any of the ABCs are compromised. Report observations to EMS. Stay with the patient. If trained, perform CPR.
Myocardial Infarction (Heart Attack)
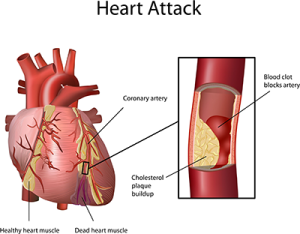
A myocardial infarction, also known as a heart attack, is a situation when the heart loses adequate oxygen supply. A myocardial infarction is a medical emergency and help must be obtained immediately.
Signs of a heart attack:
- Chest pain
- Pain that radiates (extends) to the jaw, arm, or back
- Nausea, vomiting
- Intense chest pressure (a feeling of heaviness and pressure)
- Diaphoresis (intense sweating)
- The patient clutches their chest
- Dyspnea (difficulty breathing)
- Shortness of breath
- Cyanosis (blue or gray appearance of the skin)
- Indigestion or heartburn
- Cold and clammy skin
- Weak and irregular pulse
- A sense of anxiety or impending doom
What to do:
- Immediately call 911 to obtain help.
- Loosen any clothing around the patient’s neck.
- Place them in a comfortable position and encourage them to rest. Activity uses oxygen, which the heart does not have enough of during a heart attack.
- Do not give the patient anything to eat or drink.
- Observe their breathing rate and pulse. If trained to take vital signs, do so.
- If the patient stops breathing or no longer has a pulse, perform CPR if trained to do so.
- Stay with the patient until help arrives.
- Inform a supervisor as soon as possible about the incident.
- Document the situation and all steps taken to provide care.
Seizures
A seizure is disorder in which there is increased electrical activity of the brain. In some types of seizures, the person has uncontrollable muscle movements. Tonic-clonic seizures have two phases: tonic and clonic. In the tonic phase, the person’s muscles contract and spasm. In the clonic phase, the person has repeated muscle movements, and their arms, legs, and torso may jerk violently.
Signs of a seizure:
Signs of a seizure depend on the type of seizure disorder the patient has. Home Health Aides/Personal Care Aides may notice:
- Suddenly falling or dropping from a seated or standing position
- Repeated blinking of the eyes, smacking of the lips, or repeated swallowing
- The person is not able to follow commands
- Inability to swallow
- Drooling
- Repeated contractions and movements of the arms, legs, or torso
- Shaking or jerking of the body
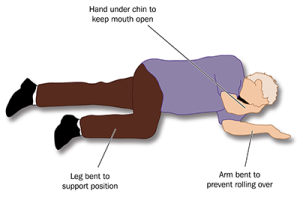
What to do:
If a patient has a seizure, it is important to obtain medical help immediately.
- Immediately call 911.
- Note the time the seizure began. Provide this information to 911.
- Place the patient in a comfortable position. Keep their head face up so they can breathe.
- Loosen any tight clothing.
- If possible, place a pillow, blanket, or towel under the patient’s head to prevent injury.
- Clear the area of any possible hazard for which the patient could become injured.
- Never put anything, including fingers, in the patient’s mouth during a seizure.
- If they begin to vomit, roll them onto their side.
- Never try to hold a patient down while they are having a seizure.
- Keep the area clear of objects and people.
- Do not give the patient food or fluid.
- Note the time when the seizure is over. Check for adequate breathing and pulse.
- If the person stops breathing or no longer has a pulse, perform CPR if trained to do so.Inform a supervisor as soon as possible about the incident.
Cerebrovascular Accident (Stroke)
A cerebrovascular accident, is also known as a stroke. A stroke can occur when the brain loses adequate oxygen supply. A stroke is a medical emergency. Obtain help immediately by calling 911.
Remember the acronym FAST when assessing someone for possible stroke.
F: Facial drooping. Is one side of the face drooping down and appear uneven?
A: Arm weakness. Can the person raise one arm or is one side weak or paralyzed?
S: Speech difficulties. Is the speech slurred or difficult to understand?
T: Time. Time is critical. If Home Health Aides/Personal Care Aides suspect a possible stroke, they should call 911 immediately!
Signs of a stroke:
- Drooping of the eye, face, or mouth
- Sudden weakness or paralysis of a hand, arm, leg, or foot. This usually occurs on one side of the body.
- Sudden inability to speak or swallow
- Tingling or numbness in an arm, hand, leg, or foot
- Sudden headache
- The patient reports suddenly having trouble seeing
- Sudden weakness
- Problems with balance, coordination
- Difficulty concentrating, remembering things
- Dizziness, fainting
What to do:
- Immediately call 911 and obtain emergency assistance.
- Keep the person in a comfortable, resting position.
- Loosen any tight clothing.
- Do not give the patient any food or liquid to drink.
Always inform a supervisor of any medical emergency. Report all injuries, no matter how insignificant (small) they seem. Always call for help for any serious medical emergency. Document all injuries and steps taken to provide care carefully and accurately. Whenever in doubt, seek guidance from a supervisor.
