Range of Motion Movements
- Abduction: moving a body part away from the midline of the body. For example, abducting the leg involves moving the entire leg away from the middle of the body.
- Flexion: bending a body part. For example, flexing a bicep involves bending it as if to make a muscle.
- Extension: straightening a body part. For example, extending a bicep involves straightening the arm.
- Pronation: turning downward. For example, the forearm and hand are turned so the palm of the hand faces downward.
- Supination: turning upward. For example, the forearm and hand are turned so the palm of the hand faces upward.
- Dorsiflexion: bending backward. For example, the toes are gently pushed towards the body to stretch the foot.
- Plantar flexion: pressing downward. For example, the toes are gently pressed down toward the sole of the foot.
- Opposition: touching the thumb to each finger. In opposition, each finger of the hand is gently moved toward the thumb to provide a gentle stretch of the hand and finger joints.
- Circumduction: making a circle with the joint. For example, circumduction of the shoulder involves the entire arm and shoulder moving in a large circle to gently exercise the joint and improve a person’s ability to move their arm and shoulder.
Many patients may be on supplements such as calcium and vitamin D, which help to support healthy muscles and bones. Be aware of fall risks by keeping items out of the patient’s path of walking, using assistive devices such as canes and walkers correctly, ensuring the patient has on non-skid shoes, and is wearing glasses and hearing aids so the person can see and hear what is going on around them.
Sensory System

The sensory system consists of our sense of vision (eyes), hearing (ears), smelling (nose), taste (tongue), and touch. Changes in vision can result in an increased risk of falls. Home Health Aides/Personal Care Aides must be aware of fall hazards. They should ensure their patient wears eyeglasses and keep rooms well lit. This will also help their patient to enjoy activities in which vision is important, such as reading. There are visual aids available that can enhance a patient’s reading experience such as books on tape, reading materials with large print, and magnifying glasses. They can also read to their patient if they would like. For patients who have trouble hearing, they should speak in a low-pitched voice without shouting, and ensure that they are directly in front of them when speaking. If they wear hearing aids, ensure they are in good working order with working batteries and that the patient uses them correctly. Remember, not every older patient will have vision or hearing problems.
Our sense of smell also diminishes as we age. This puts elderly people at a risk for not smelling fumes such as gas or in the case of fire, smoke. Home Health Aides/Personal Care Aides should ensure smoke detectors and carbon monoxide detectors are in good working order. As we age, we also lose taste buds. Combined with a decreased sense of smell, this can result in a poor appetite and weight loss. Provide food choices that are appealing to the patient and find out what their preferences are about favorite foods.
The sense of touch also diminishes as we age. It is important to be cautious about extreme temperatures as an elderly patient may not be able to tell if something is too hot or too cold. Home Health Aides/Personal Care Aides should always use ice packs and heating pads as directed by the Care Plan. Never leave them on for long periods of time as it could result in frostbite or burns. They must watch the temperature of foods and drinks they serve their patient and ensure they are not too hot which could result in burns and scalds. Some older people and those with special conditions such as diabetes may also have poor circulation. This can result in lack of feeling in their feet. Inspect the patient’s feet on a regular basis and ensure they wear proper footwear to protect them from injury.
Digestive System

The digestive system starts with the mouth where we take in food and begin the process of digestion by chewing. Food moves down the esophagus into the stomach, then into the small intestine, then into the large intestine, and finally, it is eliminated through the anus. Some elderly people may have a problem with chewing or swallowing food. This could result in a safety risk if the patient chokes. If Home Health Aides/Personal Care Aides notice their patient has any difficulties with chewing or swallowing, they should report these to their supervisor. Some patients may need to be on soft or pureed diets. If a patient wears dentures, ensure they are in place prior to meals. This will help them with chewing and properly digesting their food.
The movement of food through the digestive tract may also be slowed in some older adults. This could result in constipation. Constipation means a lack of bowel movements, or a decrease in the number of bowel movements that are normal for that particular person. It may not be uncommon for some elderly people to only have a bowel movement every couple of days. Home Health Aides/Personal Care Aides should report the frequency of bowel movements to their supervisor. Some older people may need to be on a bowel regimen to help them have regular bowel movements. This may mean they need increased fiber, which is found in foods such as fruits, vegetables and whole grains, or even medications such as stool softeners. Fluid intake and exercise are also important to maintain good bowel health.
Urinary System
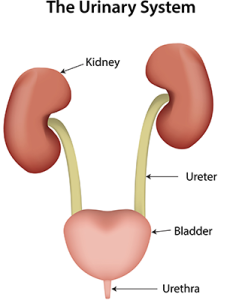
The urinary system consists of the kidneys (which make urine by filtering blood), ureters (which are tubes that carry urine from the kidneys to the bladder), the bladder (which stores urine), and the urethra (where urine passes through to the outside of the body). As we age, our kidney’s ability to filter blood decreases. Nephrons are the filtering units of the kidney. They filter waste material and make urine. The number of nephrons decreases with age. This means the ability to filter waste products decreases. Some older people may have problems with their kidneys and have to have their kidney function monitored.
The muscle tone of the bladder becomes weaker and some elderly people may have difficulty holding the same amount of urine as they did when they were younger. They may need to urinate more frequently and wake during the night to do so. Since the bladder is weaker, it may also not empty completely. This leads to urine remaining stagnant in the bladder, which makes the person more at risk for a urinary tract infection. Home Health Aides/Personal Care Aides should report any changes in urination, such as in frequency, incontinence, inability to start the flow of urine, and reports of pain or burning while urinating to their supervisor.
Encourage patients to drink plenty of fluids. Some elderly people hesitate to drink enough water because they fear they will have “an accident” or become incontinent.
Home Health Aides/Personal Care Aides should encourage them to not do this as it will only lead to dehydration and a higher chance of getting a urinary tract infection. Remember, incontinence is not a normal part of aging. They should report incidences of incontinence to their supervisor.
Endocrine System
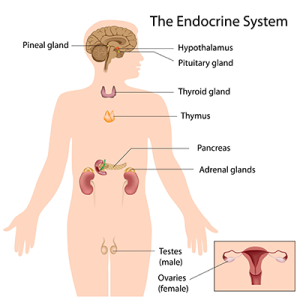
The endocrine system consists of hormones and organs such as the thyroid, parathyroid glands pancreas, and reproductive organs. The thyroid is important for metabolism. Metabolism begins to slow after the age of 20. Some older people may develop nodules on their thyroid gland and have to take medications for a thyroid gland that is overactive or underactive. The parathyroid glands, which are located near the thyroid are important to help with calcium balance. As people age, parathyroid hormone release increases. This results in too much calcium in the bloodstream and not enough calcium in the bones. This can result in weaker and more brittle bones such as that found inosteoporosis. Insulin, which is produced by the pancreas, and important for glucose (sugar) metabolism also decreases. Older patients may need to watch their sugar intake. Some elderly patients may develop diabetes. This means that the body is not producing enough insulin to allow the glucose (sugar) which we get from the food we eat to be used correctly. A supervisor and the Care Plan will direct Home Health Aides/Personal Care Aides as to whether their patient should be on a low sugar diet and if they need to monitor their blood glucose prior to meals.
The adrenal glands are located one on top of each kidney. The adrenal glands produce cortisol, which is the stress response hormone, and aldosterone, which is the hormone that regulates our fluid balance in the body. While cortisol level release decreases as we age, the amount of the hormone stays the same in the bloodstream. Elderly people are just as susceptible to stresses as any other person. High levels of stress can result in a weakened immune system and cause other physical problems, such as high blood pressure. Home Health Aides/Personal Care Aides should help their patient to eliminate stresses from their life and provide them with time to talk about what is bothering them.
As we age, aldosterone release decreases. This can result in an elderly patient having a drop in blood pressure and feeling light-headed since the body is not able to regulate its blood pressure as well. Watch for signs of light headedness anytime a patient moves from a lying down to a sitting and then standing position. Allow them a few minutes to sit and dangle their legs before they stand. This will allow their body to adjust to the changes in blood pressure.
Neurological System
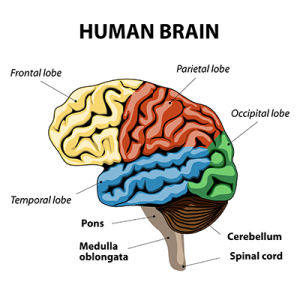
The neurological system or nervous system consists of the brain and spinal cord. Aging can result in memory loss and concentration difficulties. There is generally a slowing of nerve firing, which results in a slowing of processing information or performing tasks. Elderly people may not be able to think or perform tasks as quickly as they could before. Remember, this is not necessarily a part of aging that occurs for everyone, and it varies from person to person. Home Health Aides/Personal Care Aides should encourage their patient to make decisions and choices and to be as independent as possible. Encourage a patient to make lists to help them remember tasks. Home Health Aides/Personal Care Aides should provide plenty of time for their patient to process information and to complete tasks.
While the brain loses some nerve cells, brain connections do continue to develop.Encourage patients to think about good times by asking them about their life stories and to show photographs. Encourage and assist with activities to keep their minds active such as jigsaw puzzles, reading, crosswords, and other activities to stimulate their mental processes.
Some patients who have short-term memory loss or loss of memory about recent events can become agitated and anxious about this. Home Health Aides/Personal Care Aides should provide reassurance to them and report any changes to their supervisor so that the healthcare team is aware. If their patient shows signs of forgetfulness or confusion, they should report these to their supervisor immediately.
Female Reproductive System
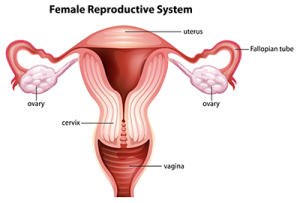
In females, a process called menopause occurs. During this time, hormone levels change as ovaries stop making estrogen and progesterone and stop releasing ova (eggs). Menstruation (otherwise known as a monthly “period”) stops during this time. Women can no longer become pregnant. As the hormone levels decrease, the vagina becomes thinner, drier, and less elastic. The labia (the external genital tissue) also becomes thinner, drier, and less elastic. These changes may be painful for some women. If a patient complains of pain in the vaginal area, Home Health Aides/Personal Care Aides should inform their supervisor.
A loss of estrogen also leads to an increased risk of osteoporosis, which is a condition in which bones become more brittle and are more at risk for fractures or breaks. There may also be an increased risk for urinary tract infections due to loss of bladder muscle tone. Loss of muscle tone in the pubic area could potentially lead to prolapsed bladder, vagina, or anus, which is a condition in which these organs drop from their original position to the outside of the body. If Home Health Aides/Personal Care Aides notice this condition, they should inform their supervisor. She will direct them about how best to care for this particular patient. There may be a diminished sexual drive due to changes in hormones and physical changes within the vagina, but this is not necessarily the case. Many elderly women continue to have sexual desires and engage in sexual activity.
Male Reproductive System
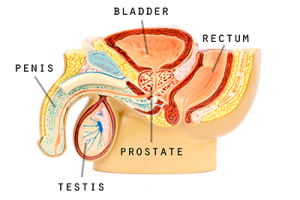
In males, testicular tissue decreases with age and there may be a decrease in testosterone, which is the male sex hormone. Testes do continue to produce sperm, but at a slower rate than before. Some men may experience erectile dysfunction, which is an inability for the penis to obtain or maintain an erection. The prostate gland becomes enlarged. The prostate gland is at the base of the bladder and around the urethra, which carries urine to the outside of the body. As it enlarges, it presses on the urethra. This can result in difficulty during urination. Men may experience dribbling, only urinating small amounts at a time, or difficulty starting or stopping the flow of urine. This is called Benign Prostatic Hypertrophy (BPH), which occurs in about 50% of men.
In some instances, an enlarged prostate may indicate prostate cancer. It is a good idea for men to be screened for prostate cancer yearly by their health care professional. This is done by what is called a DRE or Digital Rectal Exam, where the physician feels the prostate for bumps with a finger entered into the anus. Men are also screened for prostate cancer by having blood work drawn to measure levels of PSA or prostate specific antigen. Higher levels could indicate that a man has BPH or possibly prostate cancer. Decreases in sex drive may occur in some men, but this is not a definitive part of aging.
Introduction to Aging & the Mind
As we age there is generally a slowing of nerve firing, which results in a slowing of processing information or performing tasks. Elderly people may not be able to think or perform tasks as quickly as they could before. Older adults may show signs of forgetfulness, which can be normal. However, when there seem to be many memory problems and forgetfulness seems to increase, this may be a sign of a more significant problem.
There may be temporary changes in mental function that come about suddenly. Sudden changes in mental functioning and personality can be indicative of a disease process. Changes in mental function that may appear suddenly and which may be temporary can be the result of dehydration, a urinary tract infection, fever, brain infection such as meningitis, a head injury, stroke, low blood sugar levels, alcohol or substance use, and interactions or side effects from medications. If their patient has any sudden changes in their mental function, mood, or behavior, Home Health Aides/Personal Care Aides should immediately report these to their supervisor.
Working with Patients Who Have Had a Stroke

Other mental function changes that are more permanent may occur in some elderly people. A stroke, or a cerebrovascular accident can occur when there is a blockage in a cerebral artery in the brain, or if a blood vessel in the brain ruptures. Signs and symptoms of a stroke include numbness or weakness in the face or in the arms or legs, especially on one side of the body, difficulty speaking, using inappropriate words such as the wrong words for objects, and blurred vision. If Home Health Aides/Personal Care Aides notice any of these signs, they should call their supervisor immediately. Their patient may need to receive immediate medical attention.
Sometimes, the effects of a stroke are temporary and the person may regain normal functioning. In other cases, there may be permanent changes within the brain and body. Careful attention must be paid while caring for a patient after a stroke. If their patient has lost the ability to use one side of the body, they should encourage use of the stronger side by placing eating and writing utensils on the strongest side. If their patient has developed speech or swallowing problems, a Speech Therapist may become involved in the patient’s care. They will evaluate the patient’s ability to speak and to swallow. Home Health Aides/Personal Care Aides should be patient while communicating. If their patient has swallowing problems, a special diet will need to be followed and liquids may need to be thickened to prevent choking. A patient who has suffered a stroke may also have vision problems. They may only be able to see half of what is in their field of vision. Approach the patient from their stronger side, place items they need on the side they can see from, and ensure they always know what is in front of them, especially when walking.
Working with Patients with Alzheimer’s Disease

Alzheimer’s disease is a disease affecting the brain which causes permanent and progressive (continuing to get worse) changes in the brain. It is the most common cause of dementia (the loss of the ability to think, remember, reason, and plan tasks) in the elderly. Symptoms of Alzheimer’s start out typically with memory loss. As it progresses, the person becomes very confused and may forget their family, who they are, and become unable to care for themselves. They may lose the ability to communicate and may have personality changes such as aggression and withdrawal. A person with Alzheimer’s needs special care. It is important for Home Health Aides/Personal Care Aides to provide a safe environment. They may wander and end up in an unknown place with no memory of who they are, how they got to where they are, or how to go back home. It is also important to try to prevent things such as fires as a person with Alzheimer’s may begin to cook and forget they have food on the stove. Writing lists and labeling objects throughout the house may also be helpful to remind a patient with Alzheimer’s disease what the objects are. It may even be helpful to place a note on the mirror with the patient’s name or a label such as “Myself” if they are at the point where they no longer remember who they themselves are. Home Health Aides/Personal Care Aides should remember to be patient and encouraging, and find the things that seem to bring the most comfort and do these things with their patient. Many patients with Alzheimer’s enjoy music and Home Health Aides/Personal Care Aides can try playing some to help their patient relax and find enjoyment.
Working with Patients with Parkinson’s Disease
Parkinson’s disease is also a progressive and incurable disease of the mind with permanent changes. People with Parkinson’s have difficulty initiating movement, such as walking and have tremors which make it difficult to perform daily tasks such as feeding and dressing themselves. Muscles will become stiff and the person may have a shuffling gait or eventually not be able to walk at all. Dementia may occur with Parkinson’s as it progresses. When caring for a patient with Parkinson’s, Home Health Aides/Personal Care Aides should remember to be patient. It is frustrating for them to be unable to care for themselves. Encourage them to do as much as possible, and assist them with ADL’s as needed. When preparing food, keep in mind to prepare food that is easier for the patient to handle. Using adaptive eating utensils, plates, and cups can help make the eating experience more pleasurable and successful for the patient.
Introduction to Stress
A stressor is anything that causes stress. Even positive life events such as the birth of a baby or a wedding can cause people stress. Life events such as weddings, divorce, death, births of children, and retirement can cause people stress. Additional stressors affecting the elderly may include financial problems, death of a spouse, family, or close friends, physical changes, pain, and loss of independence.
When we feel stress, adrenaline is released by the endocrine system. It causes our blood pressure, heart rate, and respiratory rate to increase. Stress that is not relieved can result in long-term physical problems such as high blood pressure. It can also cause anxiety, depression, aggression, and mood swings. Some people manage stress by engaging in unhealthy behaviors such as overeating, smoking, yelling at those near them, or drinking alcohol. If Home Health Aides/Personal Care Aides observe unhealthy coping behaviors from their patient and high levels of stress, they should discuss their concerns with their supervisor and work with him or her to develop healthy coping strategies for the patient.
How to Help a Patient Effectively Manage Stress
- Encourage and provide healthy, nutritious food
- Encourage and work with the patient on maintaining physical activity or an exercise plan
- Promote good sleep by providing a peaceful sleeping environment
- Find activities the patient enjoys such as reading, listening to music, watching movies, or spending time with friends
- Teach the patient relaxation techniques such as deep breathing
- Provide a warm bath and back massage for the patient
- Apply lotion to the patient’s legs and hands If the patient wishes
- Pray with them or organize a clergy visit
- Allow the patient space to be alone for short periods to relax and think
- Provide space and time for the patient to talk and encourage them to express their thoughts and feelings
