Procedure – Assisting with Emptying of the Urinary Drainage Bag
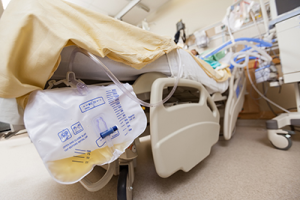
Drainage bags on urinary collection systems, such as those from indwelling catheters or condom catheters need to be emptied on a regular basis. Home Health Aides/Personal Care Aides should frequently check that the tubing on catheter systems is not twisted or kinked. Home Health Aides/Personal Care Aides should always ensure that drainage bags are below bladder level. Never hang them from bed rails as the bag will move when bed rails are raised or lowered.
- Explain the procedure to the patient.
- Wash your hands and don gloves.
- Assemble equipment needed (measuring pitcher or graduate cylinder).
- Place the measuring pitcher or graduate cylinder below the drainage bag on a paper towel.
- Release the drain from the holder.
- Open the clamp on the drainage bag without allowing the drain to touch the measuring cylinder.
- Allow contents to pour into measuring container.
- Take care to prevent urine from splashing onto your face or clothing.
- Clamp the drainage bag and clean the end of the drain with an alcohol wipe.
- Position the clamp back into its holder.
- Measure the amount of urine at eye level while it is sitting on a flat surface. Record this as output.
- Dispose of urine in the toilet. Flush. Clean the measuring container and store.
- Discard gloves and wash your hands.
- Document procedure, output, and any observed changes in behavior or condition. Report observations about changes in urine color, odor, amount, or characteristics, such as cloudiness, mucus or blood present. Note the condition of the drainage bag and catheter tubing. Report concerns or the need to replace catheter tubing or the drainage bag to a supervisor.
Procedure – Measuring Urinary Output
Fluid that is taken in must be eliminated from the body. Urine that is excreted (eliminated) from the body is called output. It is important for Home Health Aides/Personal Care Aides to measure the output of their patients to ensure optimal health. A patient may have a condition in which the healthcare provider wants to ensure that what they take in (intake) equals what they put out (output). This helps to ensure adequate fluid balance. Fluids are usually measured using milliliters (mL). The agency will specify the unit of measurement Home Health Aides/Personal Care Aides should use. Urinals and catheter drainage systems have measuring lines on the system. The amount of urine at the number indicates the amount of output. For patients who use a toilet, commode, or bedpan, urine contents can be emptied into a graduated or other measuring pitcher to provide an accurate measurement of output. Contents can be disposed of down the toilet once the urine has been measured.
- Explain to the patient the importance of measuring urinary output.
- Always wash hands and don gloves when measuring urinary output.
- Pour urine from a bedpan, commode, urinal, or urinary drainage bag into a measuring pitcher or cylinder.
- Place the measuring pitcher on a paper towel on a flat surface.
- Note amount of urine at eye level.
- Record amount. Amount of urine should be documented in milliliters (mL).
- Discard urine into toilet, unless the urine is needed for a specimen.
- If you notice anything unusual about the urine, save the urine to be inspected by a supervisor.
- Flush the toilet.
- Rinse bedpans, commodes, urinals, and measuring pitchers that have been used.
- Store equipment in the appropriate place.
- Discard gloves and wash your hands.
- Document all output.
- Report any observations or changes in condition or behavior.
- Record and report changes of characteristics of urine, including color, amount, odor, blood or mucus in the urine, or if the patient has difficulty or pain while urinating.
Introduction to Assisting with Eating
An important part of the job of a Home Health Aide/Personal Care Aide is to assist patients with eating. This may include planning and preparing meals, shopping for ingredients, serving food, and feeding.
Home Health Aides/Personal Care Aides can provide an atmosphere that is pleasant during meal time. Ensure there are no unpleasant odors. Empty trash cans, and remove urinals and bedpans from sight. Offer to assist the patient to the bathroom and to perform mouth care prior to eating. Ensure patients who wear dentures place them in their mouths prior to eating. This allows the patient to better chew and digest their food.
Patients should always be positioned in an upright position during mealtimes. This helps to prevent choking. For patients who have swallowing or choking problems, they should be kept in an upright position for 30-60 minutes once their meal is complete.
Patients with visual impairments may need to be instructed about the position of food on their plate. An easy way to do this is to use the clock method. Instruct patients about position of food using the face of a clock as a guide. For example, “The peas are at 2:00, the meatloaf is at 6:00 and the rice is at 9:00.”
Some patients may only need assistance with preparing food and are able to eat independently. Many types of adaptive equipment such as special plates, cups, and eating utensils are available to help people be as independent as possible while eating. Other patients will require complete care during eating and the Home Health Aide/Personal Care Aide will need to feed the patient. HHAs/PCAs should sit next to patients while feeding and offer to keep those who are independent eaters company. Mealtime is a good time to get to know the patient. Patients who prefer to pray or have religious or spiritual practices prior to meals should be allowed to practice these rituals. Give privacy as appropriate and requested.
Home Health Aides/Personal Care Aides should offer foods that are appealing to their patient and allow them to choose the foods they would like to eat, as appropriate. Follow ChooseMyPlate guidelines as discussed in Module 8 when selecting and preparing food to serve to patients. Follow Care Plan guidelines when preparing special diets. Refer to Module 8 for specific instruction about preparing special diets.
Procedure – Assisting with Eating
- Inform the patient that it is mealtime.
- Provide choices about foods.
- Wash and dry your hands. Always apply gloves during meal preparation and when assisting with eating.
- Assemble equipment needed (e.g. bowl, plates, cup, eating utensils, napkins).
- Allow the patient to select foods they prefer.
- Prepare the patient’s environment by ensuring there are no unpleasant odors or sights.
- Offer mouth care prior to eating. Assist with applying dentures. This allows a patient to be able to effectively chew their food. Assist or encourage the patient to put on glasses so they may see their food.
- Position the patient in a high upright sitting position. This will prevent the patient from choking or aspirating food or fluids.
- Allow the patient time to pray before eating if they wish.
- Arrange food attractively on the plate.
- Encourage the patient to do as much as they are capable. Assist only as needed.
- Cut food into small, bite-sized pieces if patient is unable to do so.
- Place a napkin under the patient’s chin. Replace soiled napkins as needed.
- Inform the patient of food temperatures, especially for food that is hot.
- Use forks and spoons gently when feeding the patient.
- Allow adequate time between bites before offering the next bite.
- Encourage the patient to chew food well before proceeding to taking the next bite.
- Mealtime is a good time for Home Health Aides/Personal Care Aides to get to know their patient. Make eating time a pleasurable experience. Be patient. Sit next to or facing the patient if assisting with feeding or while providing company during meal times. Allow the patient to eat alone if they prefer. Check on them every 5-10 minutes.
- For patients who have swallowing problems, Home Health Aides/Personal Care Aides should limit their conversation while the patients are chewing. They may need to concentrate on chewing and swallowing their food appropriately.
- Encourage, or assist, if needed, wiping of the mouth or face.Use straws or training cups as appropriate to allow ease of drinking and promotion of independence.Special plates with guards and padded eating utensils help to promote independence.
- Remove uneaten food, liquid, and soiled dishes once the patient is done eating. Clean the patient’s area and all used dishes.
- If the patient has swallowing problems, keep them in an upright position for 30-60 minutes after eating to prevent choking or aspiration of food or fluids.
- Offer hand and mouth hygiene when the patient has finished their meal.
- Remove your gloves. Wash and dry your hands.
- Document completion of the task and record any changes in condition or behavior. Report any chewing or swallowing problems. Report any changes in appetite. Record amount of food eaten and fluids taken in as intake.
Special Needs
- If the patient has a sensory impairment, such as a vision problem, tell the patient where the food is located on the plate using a clock to inform them of food position. For example, “The mashed potatoes are at the 6:00 position, the meatloaf is at 3:00 and the green beans are at 9:00.”
- If the patient has facial weakness or arm/hand weakness or paralysis, feed the patient to their strong side and/or place eating utensils on their stronger side.
- If the patient has a swallowing problem, allow longer periods between bites for adequate chewing. Limit the amount of conversation while the patient is chewing or swallowing. Ensure that the food is cut into bite sized pieces and that food is the appropriate consistency (e.g., pureed), according to the patient’s prescribed diet.
- Special plates, utensils, and cups are available to assist the patient who is weak or who has trouble grasping utensils. Eating utensils can be built up by using gauze taped around the handles.
Procedure – Measuring Intake
To maintain adequate health, we need to take in a certain amount of fluid per day. Depending on a patient’s condition, they may either be encouraged to drink fluids or limit their fluid intake. Fluid that is taken in is called intake. Fluids are usually measured using milliliters (mL). One cup of liquid is 8 ounces or 240 mL.
The amount of food that is eaten can also be measured. This can be done by weighing the food prior to serving and subtracting the amount left to get the total intake. Food intake can also be measured by determining percentage eaten. If all the meal is consumed, the intake is 100%. If none of the meal is consumed, the intake is 0%. A quarter of the meal consumed would be 25% and half the meal consumed would be 50%. The agency will specify the unit of measurement to be used.
- Explain to the patient the importance of recording their intake. Throughout your shift, ask the patient what and how much they have had to eat or drink.
- During food preparation, measure the amount of food or liquid that is served. Use standard measuring cups and spoons to properly measure intake. Record this in the appropriate place.
- Once the patient has finished eating or drinking, subtract the amount they have consumed from the amount you served. Record this number as their input. Input for fluid should be recorded as milliliters (mL).
- Record the weight or percentage of food consumed in the appropriate place.
- Document all intake. The agency may provide Home Health Aides/Personal Care Aides with a specific intake and output (I & O) sheet. They should report any observations or changes in condition or behavior.
