Immune System
The immune system becomes weaker as we age, which increases our risk for infection. This also means that it takes older people a longer time to recover from an infection. There are two parts to our immune system: the innate immune system and the adaptive immune system. As we age, changes occur in both systems. The innate immune system consists of barriers that protect us from infection, such as our skin and mucous membranes. The cough reflex and the ability to develop a fever are also part of the innate system. During the aging process, our skin becomes drier, thinner, and more fragile. More fragile skin may lead to skin tears and openings which allow bacteria to enter and cause infection. Drier skin also leads to an increased risk of cracks and openings from itching, which can allow bacteria to enter.
The adaptive immune system is more complex, and includes the spleen, thymus, tonsils, bone marrow (which makes white blood cells, which are needed to fight infection), circulatory and lymphatic systems. T cells are a type of white blood cell that helps our bodies fight infection. As we age, our body produces fewer T cells. This leads to a diminished ability to fight off bacteria and viruses. Lymph nodes reduce in size and number which makes it harder for the body to develop a fever. A fever is one way our body fights infection. An older adult may not necessarily have a fever, which is the typical sign of infection. Home Health Aides/Personal Care Aides must be aware of even slight changes in temperature as this could indicate that there is an infection. Changes in the respiratory system also lead to an increased risk of respiratory infections. As we age, our lungs have less alveoli which are needed for the exchange of oxygen and carbon dioxide. This leads to less oxygen in the blood, which means breathing may be compromised. If an older person is not able to breathe as well as they did when they were younger, they will be more at risk to contract a respiratory infection. The cough reflex may also be diminished and an older person may have a harder time coughing up mucus, which means it stays in the lungs, leading to more bacteria.
Home Health Aides/Personal Care Aides must always remember to practice good hand hygiene. It is the best way to prevent the spread of bacteria and viruses. They should assist their patient with practicing good hand and personal hygiene, and encourage and provide proper nutrition and help to keep their patient hydrated. They should encourage their patient to receive vaccinations such as a yearly influenza vaccination, and encourage them to talk to their nurse or doctor about the vaccinations they could receive to protect themselves from infection.
Respiratory System
As the body ages, there are less alveoli present in the lungs. Alveoli are small sacs at the bottom of the lungs where oxygenation takes place. The lungs take in air which contains oxygen. In the alveoli, oxygen enters the blood to oxygenate the rest of the body. Carbon dioxide, which is a waste, leaves the alveoli. Since there are less alveoli, the older person has a diminished ability to remove carbon dioxide from their lungs. Lung tissue also becomes less elastic as a person ages. This means that the lungs will not expand during breathing as well as they did when the patient was younger. The rib cage may also not expand as well as it did when the person was younger because the bones become thinner and change shape with age. The diaphragm, which is a muscle below the lungs and supports breathing also becomes weaker, so the elderly person may have a more difficult time taking deep breaths. The cough reflex may be diminished and an older person may have a harder time coughing up mucus, which means it stays in the lungs, leading to more bacteria.
When working with an older adult, Home Health Aides/Personal Care Aides should allow them to take frequent rest periods as they may become easily fatigued or short of breath. If ordered in the Care Plan, they should encourage and assist with performing deep breathing exercises. A patient may also be working with a Respiratory Therapist who will assist them with practicing deep breathing and using tools such as an incentive spirometer. An incentive spirometer is used by having the patient breathe in deeply into a small machine. This helps to keep the alveoli in the lungs open. If the alveoli are open, there will be better oxygenation of the body, and unwanted carbon dioxide can leave the body. It is also a great way to help prevent pneumonia in elderly and bedridden patients.
Some patients may benefit from staying in a higher sitting position, known as Fowler’s Position. This helps people to breathe better than if they were lying down. Home Health Aides/Personal Care Aides can adjust the patient’s bed if it is adjustable to help keep them sitting in a high position. Pillows may also be used propped behind the patient’s back to help keep them upright. They must remember to practice proper hand washing at all times. If Home Health Aides/Personal Care Aides are sick, they should talk to their supervisor about whether they should go to work or if a mask should be worn while working with patients. If they need to cough, cough away from others into the crook of the arm. Don’t cough into the hands without washing them afterward. It is important to keep the patient away from cigarette smoke and polluted air. During cold weather, ensure the patient is warmly dressed and has a scarf to cover their nose and mouth. This helps to prevent cold air from entering the lungs.
Cardiovascular System
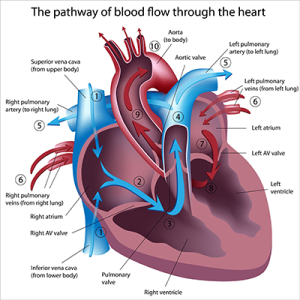
The cardiovascular system consists of the heart and all the blood vessels of the body. As we age, fatty deposits or plaque deposit in our blood vessels. These fatty deposits cause the blood vessels to become stiff and blood does not flow through them as well. If there is a large amount of plaque build-up, the flow of blood can become blocked. Coronary artery disease (narrowing of the arteries that supply blood to the heart) or heart attacks can occur due to blocked blood flow. Some people take medication to lower cholesterol levels and to prevent chest pain. Home Health Aides/Personal Care Aides should report statements of chest pain, shortness of breath, or a feeling of tightness in the chest to their supervisor immediately. The largest artery of the heart, the aorta also becomes thicker and stiffer with age. This results in many elderly people having a higher blood pressure. Monitor the patient’s blood pressure as directed in the Care Plan and report changes.
As we age, the normal rhythm of our heart also changes. Heart rate tends to decrease as we age. It is not uncommon for an elderly person to develop an arrhythmia, or an abnormal heart rhythm. In many cases this can be controlled by medications. Some patients may develop heart failure, which means the heart can no longer pump blood through the body as effectively as it used to. Patients may become short of breath, even when walking short distances or develop edema, which is a swelling of a body part, often the legs due to a build-up of water. Medications and diet changes are used to try to control the symptoms of heart failure. Home Health Aides/Personal Care Aides should report any statements made by their patient of chest pain or shortness of breath or if they notice an increase in swelling or a sudden weight gain to their supervisor immediately. These are signs that heart failure is worsening. Patients with heart failure may be told to avoid lifting heavy objects, not to engage in strenuous exercise, and to take more rest breaks while doing physical activity. Help the patient maintain as healthy a lifestyle as possible by monitoring their diet and assisting with exercise as directed in the Care Plan. Home Health Aides/Personal Care Aides should monitor for any physical changes that occur and report them to their supervisor.
Integumentary (Skin) System
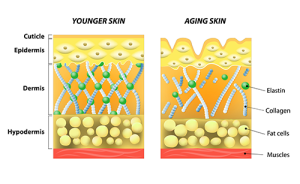
Changes in the integumentary (or skin) system may be the most visible changes of aging. Hair becomes grey and thins, and skin becomes wrinkled. Nails become harder and more brittle. The skin is the largest organ of our body. Skin serves to protect us from bacteria entering into our bodies, helps regulate our body temperature, helps us to regulate our fluid balance, and allows us to feel sensations such as heat or touch due to the nerve receptors within the skin. As we age, our skin becomes thinner, drier, and more fragile. Changes in the blood vessels within our skin also lead to the skin becoming more easily bruised and to bleeding.
As we age, sebaceous glands, which produce oil, become less active, so skin is drier, less moist, may be itchy, and is more likely to break, leading to possible infections. To protect the skin, moisture must be added, such as in the form of body lotions. It is also important to encourage older people to stay hydrated by drinking plenty of fluids. Sweat glands also become less active, so older people perspire less. They may not need a complete bath as often, but should receive a sponge bath at least daily with a complete bath about twice per week. When we sweat, it is the body’s way to keep cool. Since older people will sweat less, they are more at risk for overheating or getting heat stroke.
The subcutaneous or fat layer of the skin also thins. This leads to more difficulty with temperature regulation. Older people may become cold faster and are more at risk for developing hypothermia. Care should be taken to ensure they are properly clothed and kept warm. Thinning of the fatty layer of the skin also means that older people have less padding to protect them from injury. They may have bony areas that are at higher risk for developing pressure sores. Care should be taken to turn and position bedridden patients every two hours and to protect bony areas with pillows. In addition, it takes about 4 times longer for aging skin to heal than younger skin. In addition to the changes that occur from aging in the skin, an older patient may also have diseases and disorders such as diabetes that also prolong (lengthen) the period of time it takes for their skin and wounds to heal.
Musculoskeletal System
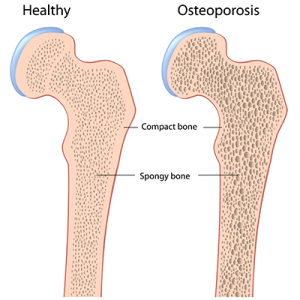
The skeleton is made up of the bones within the body. It provides support for muscles, protection for organs, and helps people to move. Muscles provide strength for the body to move. Joints are spaces in between bones, which are cushioned by cartilage and what is called synovial fluid. As people age, bones lose mass and calcium. Bones may become thinner and more likely to break. The spinal column may become curved, resulting in some elderly people having a stooped or bent over appearance. The spine is made up of vertebral disks which have fluid in between each disk. As we age, the fluid between these disks become thinner, and some people may actually lose height as this fluid thins and the vertebrae move closer together.
As people age, their muscles also weaken and lose tone. Elderly people may not have the same strength or range of motion or ROM (ability to move joints in different directions) as before and may have more difficulty with movement. Joints may become stiff, and the fluid between joints decreases, resulting in cartilage between the bones rubbing together. This makes it harder for a person to move which can be very painful. Some people have arthritis, which is painful inflammation in the joints. If safe and directed in the Care Plan, Home Health Aides/Personal Care Aides should encourage patients to perform range of motion exercises and walk as much as possible. This helps to strengthen bones and muscles, which also helps to prevent osteoporosis. Osteoporosis results in thin and brittle bones, which increases a person’s risk of fractures. Home Health Aides/Personal Care Aides can assist with range of motion (ROM) exercises as directed in the Care Plan, and can encourage patients to complete as many activities as possible to keep their muscles and bones active.
Home Health Aides/Personal Care Aides may assist with performing range of motion exercises only as directed in the Care Plan. They should never perform these types of activities without proper training and direction from their supervisor, as it could result in injury to the patient. Patient’s joints should always be supported during these types of activities. Joints can be supported by holding above and below the joint. For example, when performing exercises involving the knee, the HHA/PCA can hold the area below and above the knee joint during the activity. Patients should never be forced to do exercises that hurt. Joints should be moved slowly and gently during these exercises. Any pain should be reported to the supervisor. Remember, you must NOT perform these exercises unless you have been properly trained and directed to do so.
